Bloodshot Eye on One Side: Causes, Risks & Treatment
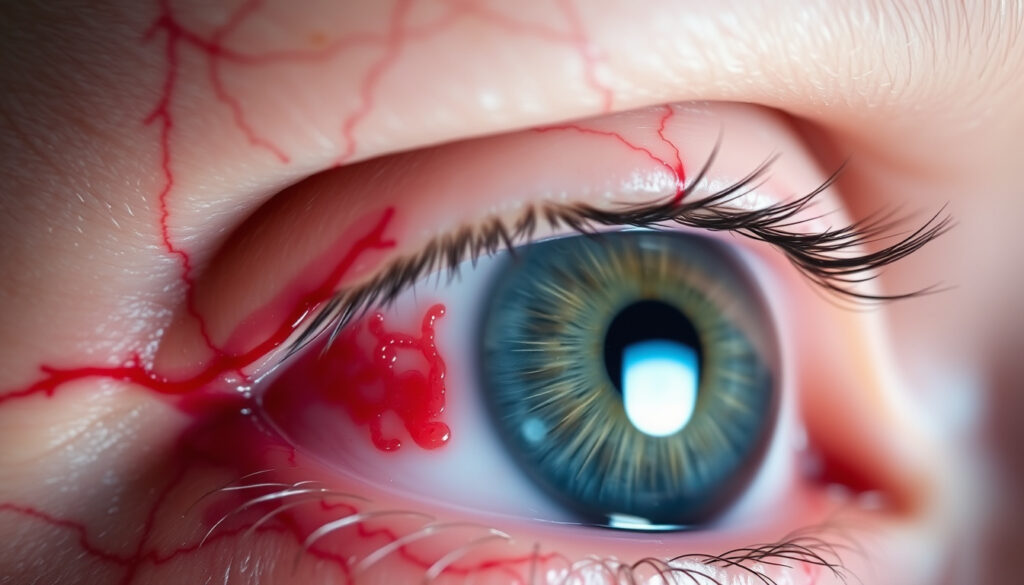
You wake up, look in the mirror, and half the white of one eye is bright red. It looks alarming — like something serious. But here is the reassuring truth most people don’t know: a sudden bloodshot eye on one side is usually a burst blood vessel under the conjunctiva, and it typically clears up on its own within 2–3 weeks. The trick is knowing when it is genuinely benign and when it signals something worth a doctor’s visit.
Most common cause: Subconjunctival hemorrhage · Usually requires: No treatment · Typical duration: 1–2 weeks · Serious if with: Pain or vision loss
Quick snapshot
- Benign in most cases (Health Service Executive)
- Subconjunctival hemorrhage common per Mayo Clinic (Mayo Clinic)
- Resolves within 2–3 weeks (Cleveland Clinic)
- Exact stroke risk without other symptoms
- Whether isolated SCH ever serves as a standalone warning sign
- Mechanisms behind recurring cases in otherwise healthy individuals
- Most cases self-resolve with no treatment
- Artificial tears for minor irritation
- See an eye doctor if redness persists beyond 3 weeks or recurs
Key clinical markers separate routine cases from those requiring professional evaluation.
| Factor | Details |
|---|---|
| Primary Symptom | Redness in one eye only |
| Top Cause | Broken blood vessel (subconjunctival hemorrhage) |
| Urgency | Usually low; monitor for additional symptoms |
| Duration | 7–14 days for most cases |
| Common Triggers | Straining, eye rubbing, contact lenses, blood pressure spikes |
| At-Risk Medications | Warfarin, aspirin, interferon |
Why is my eye randomly bloodshot on one side?
A bloodshot eye that appears out of nowhere on just one side typically points to subconjunctival hemorrhage (SCH) — a broken blood vessel sitting under the clear membrane that covers the white of your eye. It looks dramatic, but the underlying cause is usually mundane: something as simple as vigorous coughing, sneezing, vomiting, or even rubbing your eye too hard can burst a tiny vessel.
The hallmark of this condition is that it is painless and does not affect your vision. According to the Cleveland Clinic (authoritative medical center), SCH typically resolves on its own within 2–3 weeks without any lasting effects. The red patch you see is blood trapped under the conjunctiva — not inside the eye itself — so it cannot damage your sight.
Common causes like subconjunctival hemorrhage
The Mayo Clinic identifies several everyday triggers:
- Straining — coughing, sneezing, vomiting, constipation, or heavy lifting
- Physical irritation — rubbing your eye, wearing contact lenses that fit poorly
- Sudden pressure spikes — a sharp rise in blood pressure
- Trauma — direct injury to the eye area
In younger patients, trauma and contact lens usage represent the leading risks, while in older adults, underlying vascular conditions like hypertension, diabetes, and arteriosclerosis play a larger role, per research published in PMC NCBI (peer-reviewed medical literature). Blood-thinning medications including warfarin, aspirin, and interferon also increase susceptibility.
Infection or allergy triggers
Unilateral redness more often stems from local irritation rather than systemic allergy. If both eyes were affected, allergies or viral conjunctivitis would be more likely suspects. A single eye going red without discharge or itching points toward SCH rather than infection, according to Eduardo Bessermd (board-certified ophthalmologist).
The absence of pain, discharge, or vision change tells you the redness is likely superficial. An infection, by contrast, typically brings itching, mucus, or a gritty sensation.
When only one eye turns red without systemic signs, the diagnosis typically points to a mechanical cause rather than infection.
What causes sudden redness in one eye?
Sudden redness in one eye without warning usually means a small blood vessel under the conjunctiva has ruptured. The WebMD health team explains that irritated or dilated blood vessels cause the telltale red patch. Unlike redness from dryness or allergies, SCH appears as a sharply defined bright-red spot that can spread slowly over 24–48 hours before beginning to fade.
“Anything causing a sudden pressure spike — violent coughing fits, childbirth, heavy weightlifting, or severe constipation — can rupture conjunctival vessels.” — Cedars-Sinai (academic medical center)
Trauma or strain
Physical strain is the most common trigger. Cedars-Sinai notes that anything causing a sudden pressure spike — violent coughing fits, childbirth, heavy weightlifting, or severe constipation — can rupture conjunctival vessels. Direct trauma from an object or blow also produces localized bleeding at the injury site.
Spontaneous burst
Sometimes the burst happens with no identifiable cause. Your vessel wall may simply be weaker at that point, or a momentary blood pressure elevation you did not notice triggered it. The Health Service Executive (Ireland’s public health service) reassures patients that the condition usually improves on its own without intervention.
The pattern here is clear: most sudden red eyes trace back to mechanical pressure, not underlying disease.
When should I worry about a bloodshot eye?
Most unilateral bloodshot eyes are harmless, but certain signs demand professional attention. The Cleveland Clinic advises seeking immediate care if you experience pain, vision changes, unusual light sensitivity, or blood pooling in front of the iris — the last symptom suggests hyphema, a potentially serious bleeding episode inside the eye itself.
SCH alone is not dangerous. But if pain, vision loss, or blood inside the colored part of your eye accompanies the redness, treat it as urgent. These symptoms point to conditions requiring prompt evaluation.
Signs needing doctor visit
Contact an eye care provider if redness persists beyond 2–3 weeks, recurs frequently, or is accompanied by any of these warning signs per WebMD:
- Pain or tenderness in the eye
- Vision blurring or loss
- Light sensitivity
- Discharge or crusting
- Redness that worsens after 48 hours
- History of bleeding disorders or blood thinners
Painless vs painful
Pure SCH is painless by definition. If your red eye hurts, something else is at play — a scratched cornea, uveitis, acute glaucoma, or infection. Pain transforms a routine occurrence into something requiring diagnosis. Eduardo Bessermd emphasizes that isolated painless redness is reassuring, while painful redness warrants evaluation within 24–48 hours.
“Isolated painless redness is reassuring, while painful redness warrants evaluation within 24–48 hours.” — Eduardo Bessermd (board-certified ophthalmologist)
The key takeaway: pain flips a routine event into something that needs professional assessment.
Does a broken blood vessel in the eye indicate a stroke?
This is the question that frightures most people who wake up with a red eye: is this a warning sign of stroke? Here the medical evidence tells a split story — one study flagged a connection, but a larger, more recent analysis challenges it.
Stroke symptoms to watch
Stroke from a broken blood vessel in the eye is extremely rare. Real stroke symptoms involve more than the eye — sudden weakness or numbness on one side of the body, difficulty speaking, facial drooping, or severe headache. Per Eduardo Bessermd, SCH alone is not diagnostic for stroke. Eye redness in isolation does not constitute a stroke warning.
Differences from hemorrhage
A 2011 Taiwanese nationwide study found that patients with conjunctival hemorrhage carried a 1.33 hazard ratio for stroke within 3 years — an incidence of 2.44 versus 1.63 per 100 person-years in controls, according to research published in Wiley Online Library (peer-reviewed ophthalmology journal).
However, a 2021 Korean nationwide cohort study published on November 18, 2021, reached a different conclusion: after adjusting for confounders like age, hypertension, and diabetes, SCH patients showed a 10-year stroke/MI probability of 3.17% versus 2.71% in matched controls — a difference not statistically significant, per Review of Optometry (specialist optometry publication).
Both conditions share risk factors — age, hypertension, diabetes — which likely explains the earlier association. The Korean study’s adjustment for these confounders largely dissolves the link.
The Review of Optometry reports that clinicians should reassure patients that SCH does not independently increase stroke risk. The Refocus Eye Doctors practice adds that stopping blood thinners over SCH concerns risks far worse outcomes — the preventive benefit against heart attack and stroke outweighs the minor inconvenience of eye bleeding.
How long will it take for a bloodshot eye to go away?
The timeline is predictable: the red patch grows over the first 24–48 hours, then gradually fades as your body reabsorbs the trapped blood. Most cases clear within 2–3 weeks, according to Cleveland Clinic. Yellowing may appear briefly as the blood breaks down — this is normal and not a sign of infection.
Healing timeline
Expect these stages per WebMD:
- 0–48 hours: Red patch may spread or intensify
- Days 3–7: Peak redness; gradual stabilization
- Week 2: Fading begins; possible yellow tint
- Weeks 2–3: Complete resolution in most cases
Home care tips
No special treatment is usually required. The Cleveland Clinic recommends artificial tears to address any minor irritation. Avoid rubbing your eye, and skip contact lenses until the redness fully resolves. If you take blood thinners, do not stop them — the stroke-prevention benefit outweighs the SCH risk, per Refocus Eye Doctors.
Recurrent SCH warrants checking your blood pressure and, if on warfarin, your INR levels. Frequent unexplained bursts may signal an underlying vascular issue worth investigating.
For most people, the eye heals itself — but repeated episodes deserve medical follow-up.
Related reading: Skin Cancer on Nose · What Bed Bug Bites Look Like
While subconjunctival hemorrhage remains common, pink eye symptoms frequently include the unilateral redness that signals possible infection or irritation.
Frequently asked questions
What is subconjunctival hemorrhage?
Subconjunctival hemorrhage (SCH) is a broken blood vessel under the clear membrane covering the white of your eye. It creates a bright red patch that looks alarming but is typically painless and harmless, resolving within 2–3 weeks.
Can allergies cause bloodshot eye on one side?
Allergies more commonly affect both eyes. Unilateral redness without itching or discharge points toward SCH rather than allergy. If both eyes itch and water simultaneously, allergies or viral conjunctivitis are more likely culprits.
Is bloodshot eye on one side contagious?
SCH is not contagious — it is a mechanical rupture of a blood vessel, not an infection. Viral or bacterial conjunctivitis, by contrast, spreads easily through hand-to-eye contact.
What home remedies help bloodshot eyes?
Artificial tears soothe any irritation. A cool compress can ease discomfort. Avoid eye rubbing, and pause contact lens wear until the redness clears. No other intervention is typically needed.
Can stress cause a bloodshot eye?
Stress alone does not cause SCH, but it can raise blood pressure, which may contribute to vessel rupture in susceptible individuals. The direct triggers remain physical: straining, rubbing, or pressure spikes.
Does bloodshot eye affect vision?
Typical SCH does not impair vision. If you notice blurring, double vision, or loss of visual acuity alongside redness, see a doctor promptly — these symptoms suggest a more serious condition.
Can dry eyes cause one-sided redness?
Dry eye syndrome causes bilateral redness more often. SCH from dry eye rubbing is possible but less common than the direct straining or trauma triggers listed above.
For anyone on blood thinners who develops frequent or unexplained SCH, the practical next step is a conversation with your prescribing physician about INR monitoring or dosage review — not stopping the medication outright. The PMC NCBI guidance notes that recurrent SCH in patients sharing stroke risk factors warrants evaluation for underlying vascular disease.